Potential Reversal of Alzheimer’s Disease
Dr. Dale Bredesen, professor at both the Buck Institute for Research on Aging and at the Easton Laboratories for Neurodegenerative Research at UCLA, announced that he may have found a potential treatment for the reversal of memory loss associated with Alzheimer’s disease. The push for a cure for Alzheimer’s is strong as over 5.4 million Americans currently live with the disease.
 Published in the journal Aging, Bredesen and his research team studied ten people who were experiencing age-related memory loss. Nine of the ten participants had genetic mutations in the APOE4 gene associated with Alzheimer’s disease, putting them at high risk. Participants used a technique called metabolic enhancement for neurodegeneration (MEND), a 36-point personalized regimen focused on a healthy diet, exercise routine, brain stimulation, sleep improvements, medication and vitamins for 5 months to 2 years.
Published in the journal Aging, Bredesen and his research team studied ten people who were experiencing age-related memory loss. Nine of the ten participants had genetic mutations in the APOE4 gene associated with Alzheimer’s disease, putting them at high risk. Participants used a technique called metabolic enhancement for neurodegeneration (MEND), a 36-point personalized regimen focused on a healthy diet, exercise routine, brain stimulation, sleep improvements, medication and vitamins for 5 months to 2 years.
Using magnetic resonance imaging (MRI) brain scans and neuropsychological testing, the team was able to assess the success of the customized programs for each individual. They found that the MEND technique drastically improved the lives of the participants: those that had to leave work due to their memory decline were able to return, and others who had reported struggling with work saw an improvement in performance.
The hippocampus, a critical brain region for learning and memory, often shrinks in individuals with Alzheimer’s. At the beginning of the study, one patient’s hippocampal volume was in the 17th percentile for his age range, but after following the MEND program for 10 months, this specific participant’s hippocampal volume increased drastically to the 75th percentile.
Health care professionals agree that a personalized approach to brain health is the best way to prevent and delay signs of cognitive decline. However, not all scientists support the MEND approach, as it includes treating conditions that could be associated with Alzheimer’s, such as inflammation, and incorporates supplements that are not well studied or do not require FDA approval.
Bredesen hopes to further prove that treating the underlying causes and mechanisms of the disease will help reverse symptoms. So far, his efforts have proved valid, though a larger sample size and longer study would further validate the effectiveness of the program.
In line with Bredesen’s approach, the Cognitive Therapeutics Method™ is a personalized, one-on-one program designed to keep aging minds sharp. The Method is customized to each client’s unique needs and offers a range of activities that are fun yet just challenging enough to keep the brain engaged, thereby possibly delaying symptoms of cognitive decline. The Method has been an integral part of Home Care Assistance’s approach to brain health for seniors over the past three years.
To learn more about the Method, visit www.HomeCareAssistance.com/Cognitive-Therapeutics-Method today.
Sources
http://www.impactaging.com/papers/v8/n6/abs/100981a.html
http://www.cbsnews.com/news/can-memory-loss-in-alzheimers-patients-be-reversed/

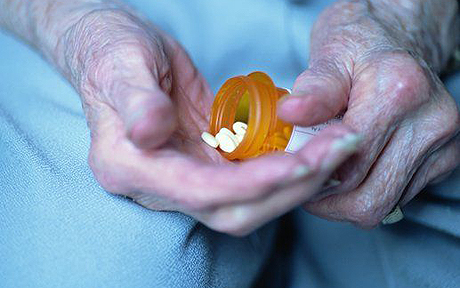 Popular heartburn drugs, such as Prilosec and Nexium, were recently linked to an increased risk of dementia in a study published in JAMA Neurology. Heartburn drugs are known as proton pump inhibitors (PPIs) because they reduce acid production by blocking the enzyme in the stomach that produces it. PPIs have long been linked to kidney problems, bone fractures and more, and now research has uncovered that PPI drugs are associated with cognitive decline as well.
Popular heartburn drugs, such as Prilosec and Nexium, were recently linked to an increased risk of dementia in a study published in JAMA Neurology. Heartburn drugs are known as proton pump inhibitors (PPIs) because they reduce acid production by blocking the enzyme in the stomach that produces it. PPIs have long been linked to kidney problems, bone fractures and more, and now research has uncovered that PPI drugs are associated with cognitive decline as well. Described as encouraging by the research community, these results prove that a CSF1R treatment could be a potential therapy option for treating Alzheimer’s disease. Further studies will be needed to verify the long-term effectiveness of the drug in humans.
Described as encouraging by the research community, these results prove that a CSF1R treatment could be a potential therapy option for treating Alzheimer’s disease. Further studies will be needed to verify the long-term effectiveness of the drug in humans.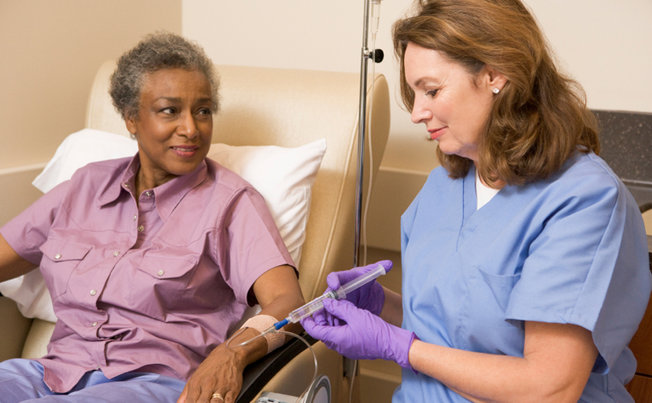 The study, published in JAMA Oncology, compared the effects of anthracycline, a commonly prescribed chemotherapy agent, with non-anthracycline agents in breast cancer survivors. The participants had been off of their treatments for more than two years and were an average age of 55 years old. Twenty women received anthracycline-based treatments, nineteen received non-anthracycline-based treatments and twenty-three did not receive chemotherapy at all.
The study, published in JAMA Oncology, compared the effects of anthracycline, a commonly prescribed chemotherapy agent, with non-anthracycline agents in breast cancer survivors. The participants had been off of their treatments for more than two years and were an average age of 55 years old. Twenty women received anthracycline-based treatments, nineteen received non-anthracycline-based treatments and twenty-three did not receive chemotherapy at all.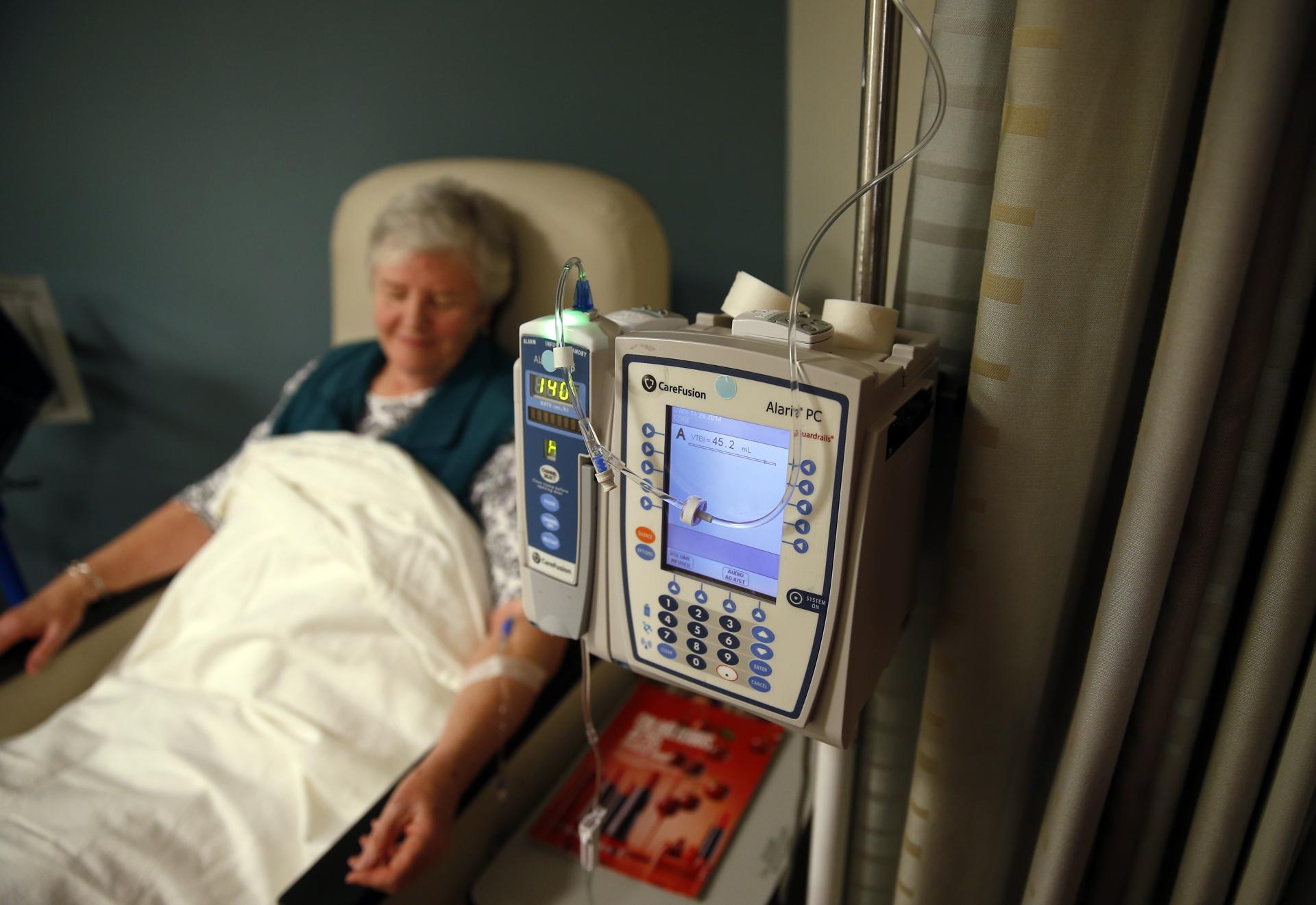 The A4 trial is taking place in 60 hospitals that are looking for 1,000 patients to test solanezumab, a monoclonal antibody with a high safety profile that clears out amyloid beta proteins. They are hoping to find individuals like Helene DeCoste of Boston, a current patient in the clinical trial. Helene is an ideal candidate because she has no sign of memory loss yet but brain scans reveal a build-up of amyloid plaque in her brain, a hallmark of Alzheimer’s disease. Dr. Reisa Sperling, a physician at Harvard University and project director of the A4 study, spoke of Helene DeCoste as “a perfect patient for this trial“.
The A4 trial is taking place in 60 hospitals that are looking for 1,000 patients to test solanezumab, a monoclonal antibody with a high safety profile that clears out amyloid beta proteins. They are hoping to find individuals like Helene DeCoste of Boston, a current patient in the clinical trial. Helene is an ideal candidate because she has no sign of memory loss yet but brain scans reveal a build-up of amyloid plaque in her brain, a hallmark of Alzheimer’s disease. Dr. Reisa Sperling, a physician at Harvard University and project director of the A4 study, spoke of Helene DeCoste as “a perfect patient for this trial“. Biogen Idec, a pioneer in the biotech industry that develops treatments for neurodegenerative diseases and other medical conditions, made news last Friday when it announced the success of a new drug for Alzheimer’s disease. The PRIME study demonstrated positive results of aducanumab in patients with pre-onset symptoms and mild-Alzheimer’s disease, which represents an outstanding breakthrough in Alzheimer’s research.
Biogen Idec, a pioneer in the biotech industry that develops treatments for neurodegenerative diseases and other medical conditions, made news last Friday when it announced the success of a new drug for Alzheimer’s disease. The PRIME study demonstrated positive results of aducanumab in patients with pre-onset symptoms and mild-Alzheimer’s disease, which represents an outstanding breakthrough in Alzheimer’s research.